НАШИ УСЛУГИ

Public Relations (PR)
Работа над повышением интереса журналистов к деятельности компании, продвижение брендов и персон, публикации в СМИ. Антикризисный PR

Корпоративные СМИ
Разработка корпоративных изданий «под ключ». Концепция; разработка дизайна; подготовка текстов; верстка; полная предпечатная подготовка

Дизайн и креатив
Создание креативных концепций; разработка фирменного стиля и дизайн-макетов полиграфической продукции. Нейминг. Видеопродакшн

Тексты и статьи
Создание уникального контента сайта, написание качественных текстов для полиграфии. Подготовка статей, интервью, репортажей, новостных текстов
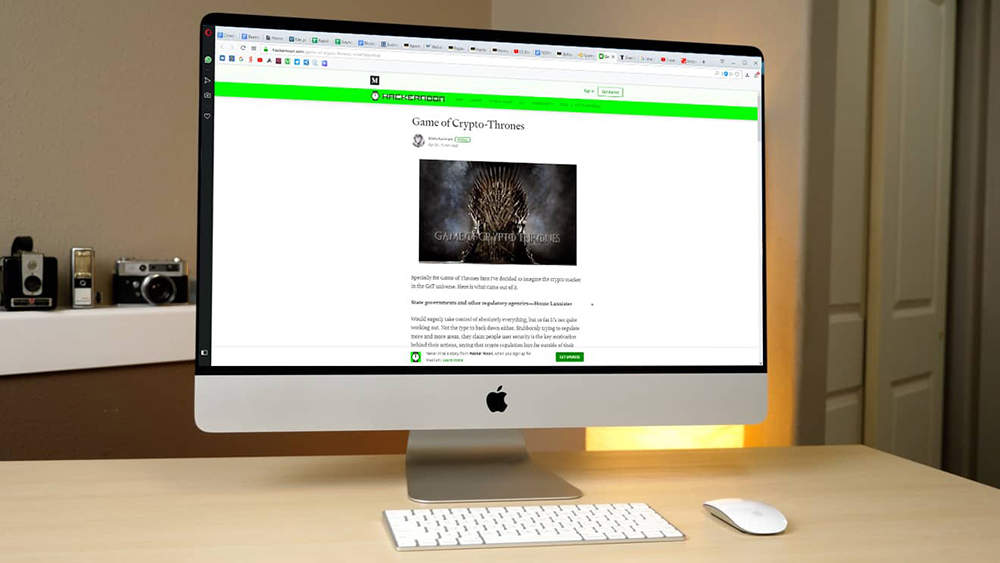
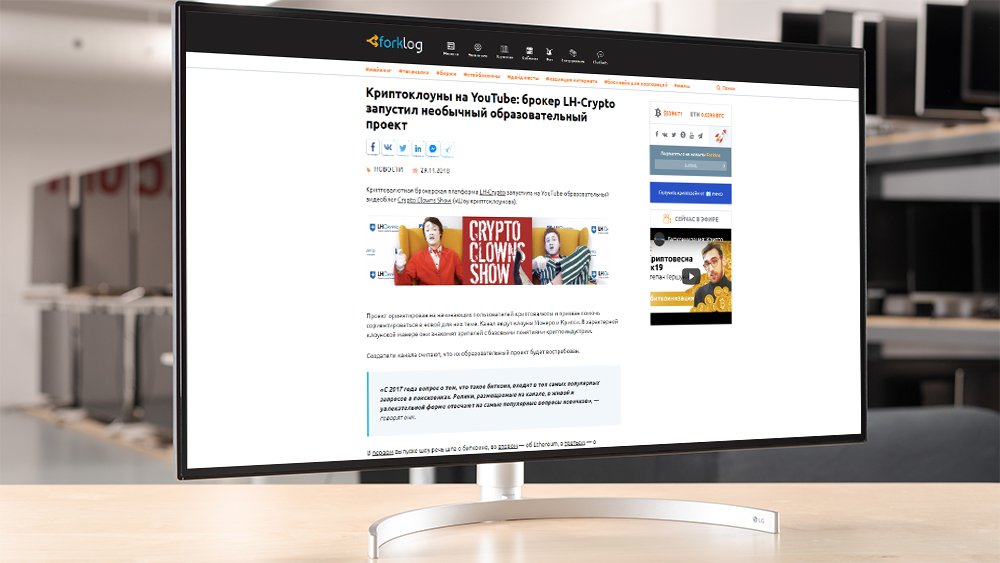
Blockchain и крипто-проекты
DIGITAL НАПРАВЛЕНИЕ

Поисковая оптимизация (SEO)
Продвижение вашего сайта, улучшение позиций в поисковой выдаче. Работа с кодом, текстами, версткой. Наращивание внешних факторов

Digital-маркетинг
Полный комплекс услуг по интернет-рекламе, от индивидуальной настройки стратегии, до создания баннеров и покупки ссылок и статей

Социальные сети (SMM)
Ведение групп в социальных сетях, блогов и веток на форумах. Создание текстового и графического контента. Комьюнити менеджмент
Наши проекты
- Все
- КОРПОРАТИВНЫЕ СМИ
- ДИЗАЙН И КРЕАТИВ
- ТЕКСТЫ
- PR
- SMM